The outcome may say more about AI than anyone expected.
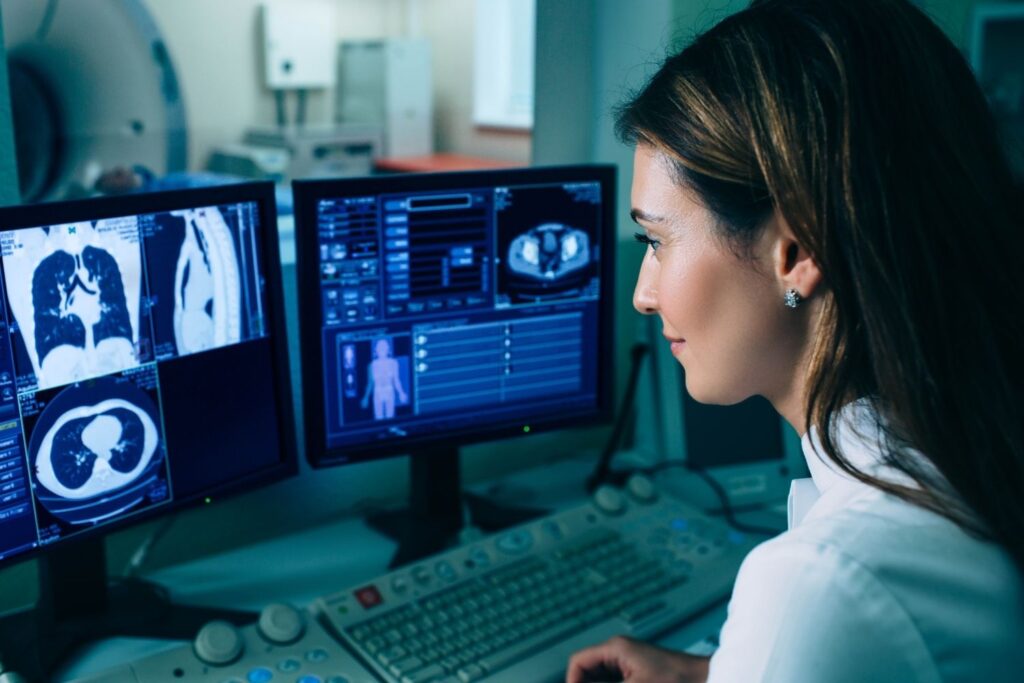
For years, experts predicted that certain high skill professions would be among the first to fall to artificial intelligence. The tools arrived quickly, the data sets expanded, and the forecasts sounded confident. But inside one critical field, the results have been more complicated. Algorithms perform impressively in controlled settings, yet real world decisions continue to resist full automation. As researchers examine outcomes more closely, a pattern is emerging that raises uncomfortable questions about what machines can do, and what they still cannot replicate.
1. Radiology became the frontline of AI medicine.
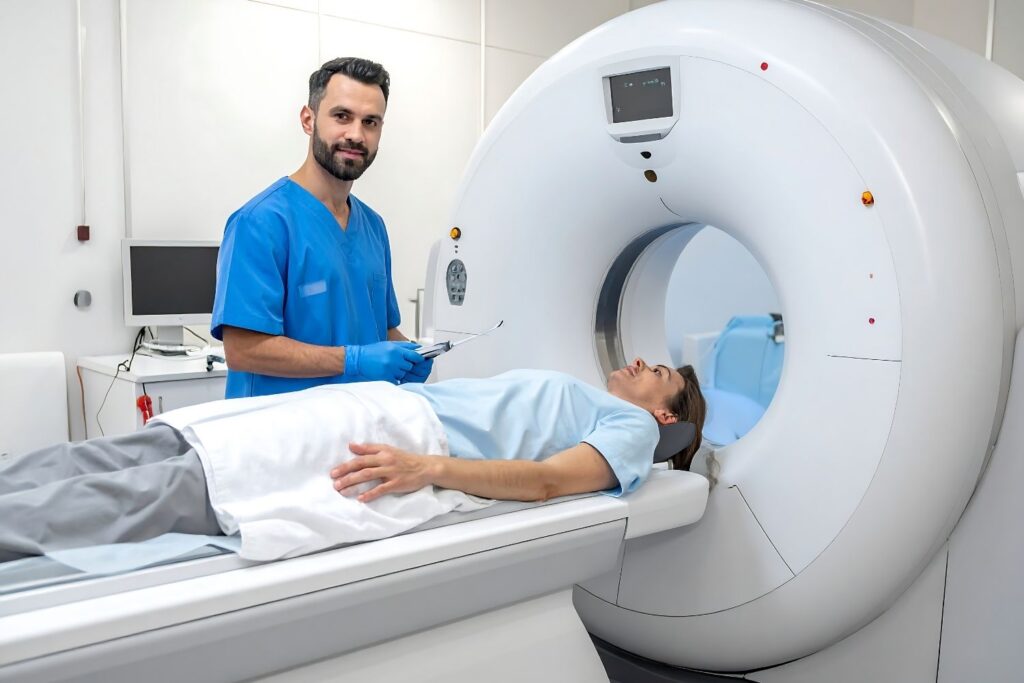
By the mid 2010s, AI systems were already outperforming average readers in narrow image recognition tasks. Headlines predicted that radiologists would soon be replaced entirely. According to The New England Journal of Medicine, early deep learning models demonstrated remarkable accuracy in detecting specific abnormalities in controlled studies.
That performance created urgency within healthcare systems. Yet radiologists quickly pointed out that clinical medicine rarely mirrors laboratory benchmarks. The challenge is not spotting a pixel anomaly alone, but integrating findings into a broader patient context where ambiguity is constant.
2. Diagnostic imaging involves layered clinical judgment.
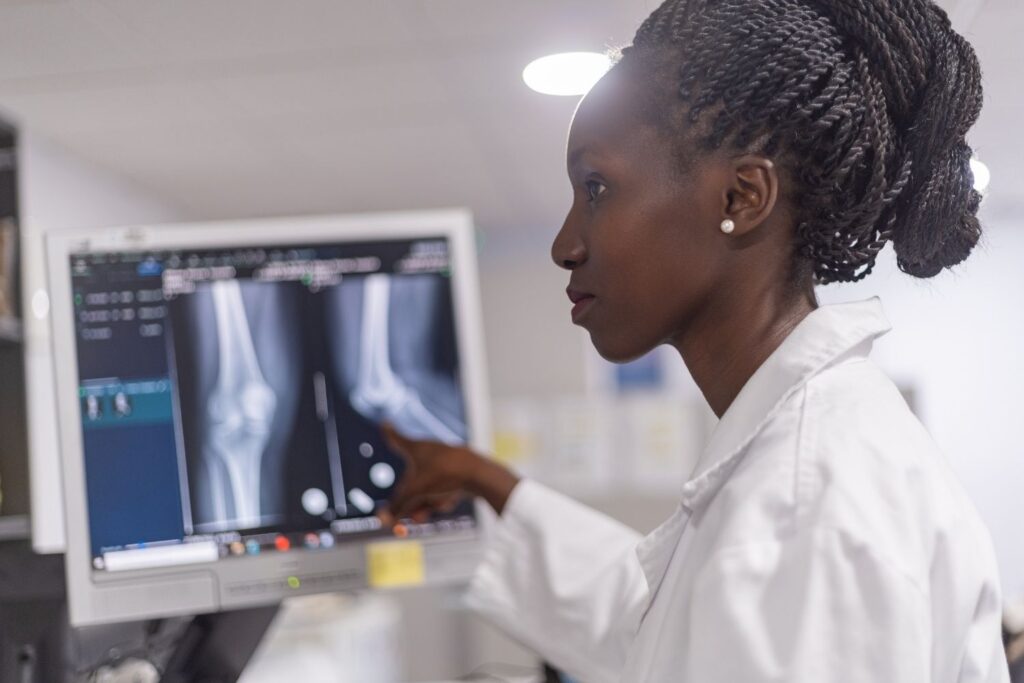
A radiologist does more than identify shadows on a scan. Each interpretation is shaped by patient history, laboratory data, symptoms, and prior imaging.
As reported by The Lancet Digital Health, AI tools often excel in single task pattern recognition but struggle when multiple overlapping conditions complicate interpretation. Radiologists routinely weigh competing explanations, incidental findings, and incomplete information. That layered reasoning extends beyond what current models consistently handle in real world clinical environments.
3. Errors reveal limits of autonomous systems.

AI systems trained on curated datasets can falter when exposed to unfamiliar imaging artifacts or demographic variation. Real world deployment exposes these vulnerabilities.
According to the American College of Radiology, oversight remains essential because algorithms may misclassify rare conditions or fail under atypical imaging parameters. Human radiologists detect when data looks inconsistent or suspicious. They adjust for equipment differences, patient movement, or subtle anomalies that fall outside standardized training sets.
4. Radiologists integrate communication and ethics.

Imaging results do not exist in isolation. Radiologists consult with surgeons, oncologists, and emergency physicians, explaining uncertainty and recommending next steps.
They must also weigh ethical implications, such as incidental findings that could trigger invasive procedures. These discussions require empathy, contextual awareness, and professional accountability, qualities not reducible to image analysis alone.
5. Liability remains anchored to human oversight.
In clinical practice, responsibility for diagnostic decisions rests with licensed physicians. Hospitals and insurers require accountable professionals who can justify interpretations.
Even when AI assists in screening, radiologists sign reports and assume legal liability. That framework reinforces the necessity of human expertise until regulatory systems redefine responsibility, a shift that remains unresolved in many jurisdictions.
6. Complex cases demand adaptive reasoning.
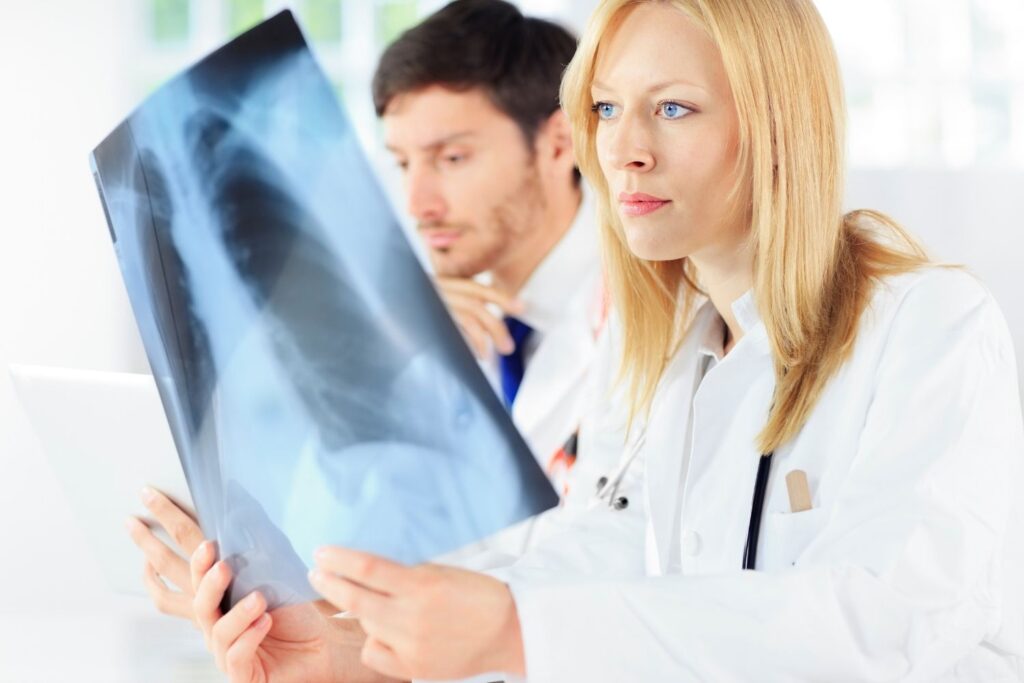
Cancer staging, trauma assessment, and rare disease identification often require synthesizing multiple imaging modalities. Radiologists compare CT, MRI, ultrasound, and patient progression over time.
Adaptive reasoning allows them to update interpretations as new information emerges. AI systems trained for fixed outputs can struggle with dynamic reassessment, particularly when new variables enter unexpectedly.
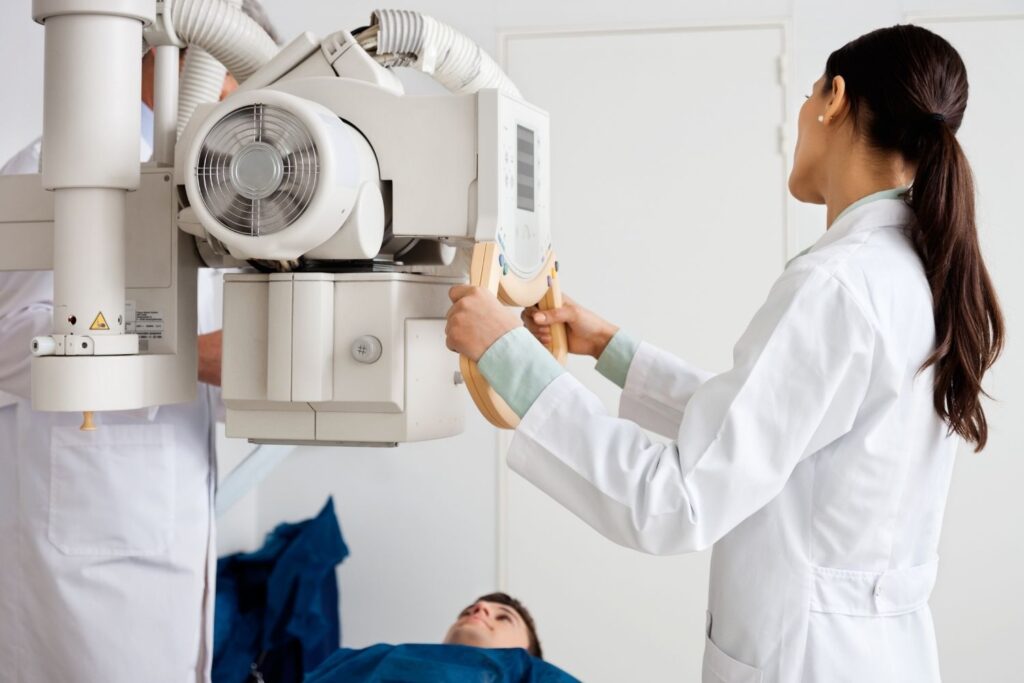
7. Training pipelines continue to expand.
Despite predictions of job loss, radiology residency programs in the United States remain competitive. Enrollment has not collapsed.
Medical students recognize that AI tools are becoming integrated assistants rather than replacements. Radiology education now includes instruction on evaluating algorithm performance, reinforcing a collaborative rather than adversarial relationship between physician and machine.
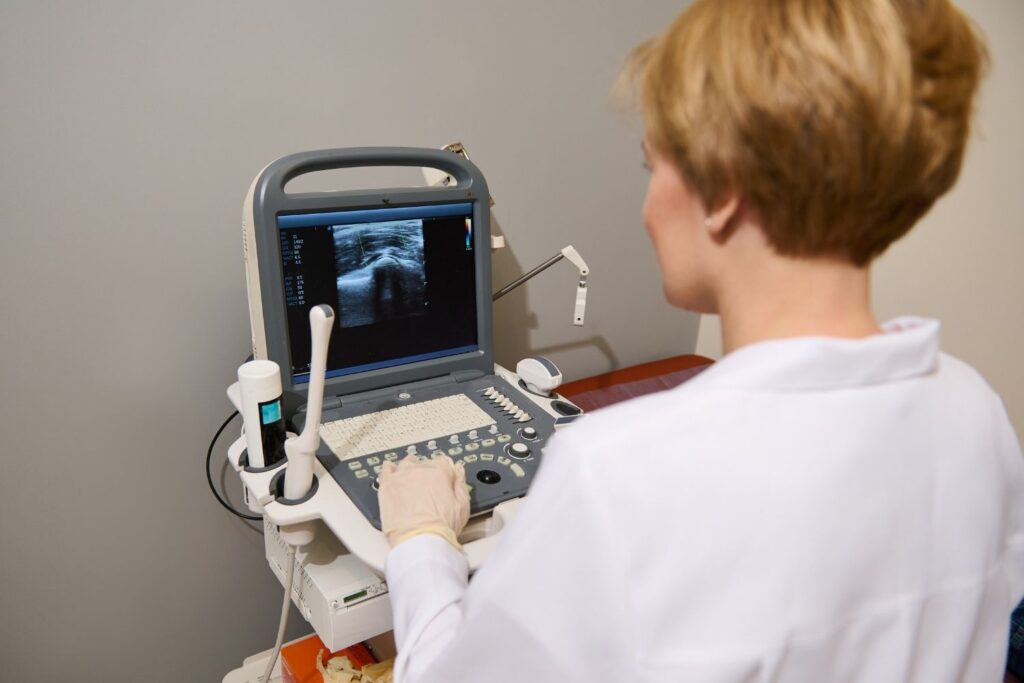
8. Algorithms require constant recalibration.
Imaging equipment evolves, disease prevalence shifts, and population demographics change. AI models must be retrained regularly to maintain performance.
Radiologists participate in validation studies and quality assurance processes to ensure safe deployment. Without continuous oversight, algorithm accuracy can degrade, particularly when applied outside original training conditions.
9. Human intuition detects subtle narrative shifts.
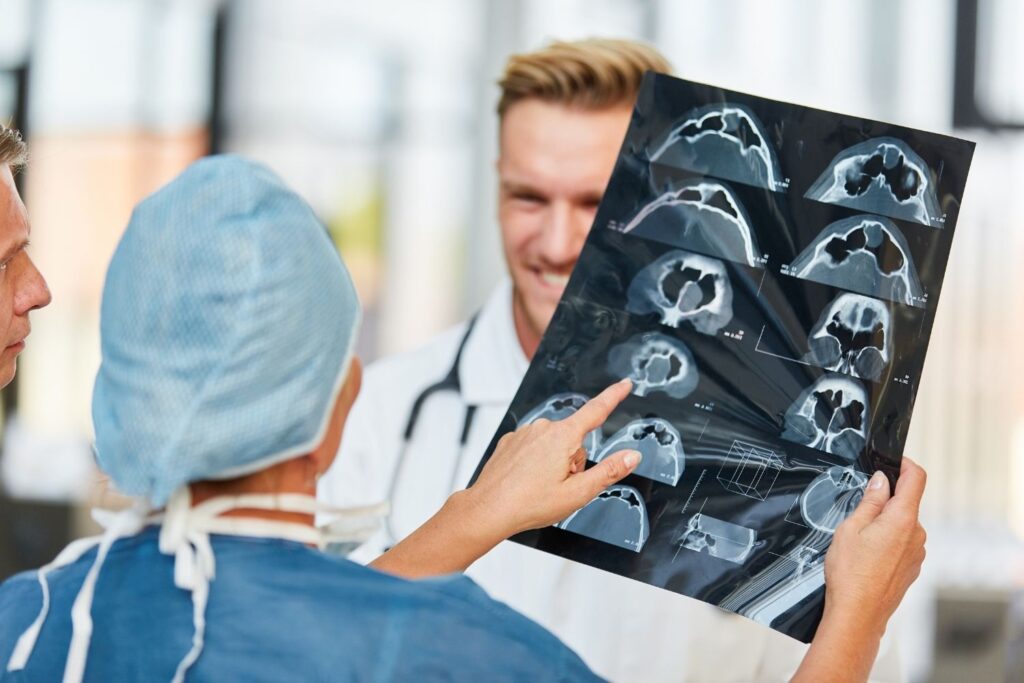
Experienced radiologists often sense patterns that do not conform neatly to statistical categories. They notice subtle contextual cues, such as patient anxiety or symptom progression.
This intuitive layer, built through years of exposure, helps prevent premature conclusions. While AI can flag abnormalities, determining clinical significance often depends on interpretive nuance shaped by accumulated human experience.
10. The field evolved instead of disappearing.

Rather than vanishing, radiology has absorbed AI into workflow. Automated triage systems prioritize urgent scans, allowing radiologists to focus on complex cases.
This integration demonstrates that advanced automation does not necessarily eliminate professional roles. Instead, it can redefine them. Radiology now stands as a test case for how artificial intelligence interacts with expertise, oversight, and accountability in high stakes environments.
